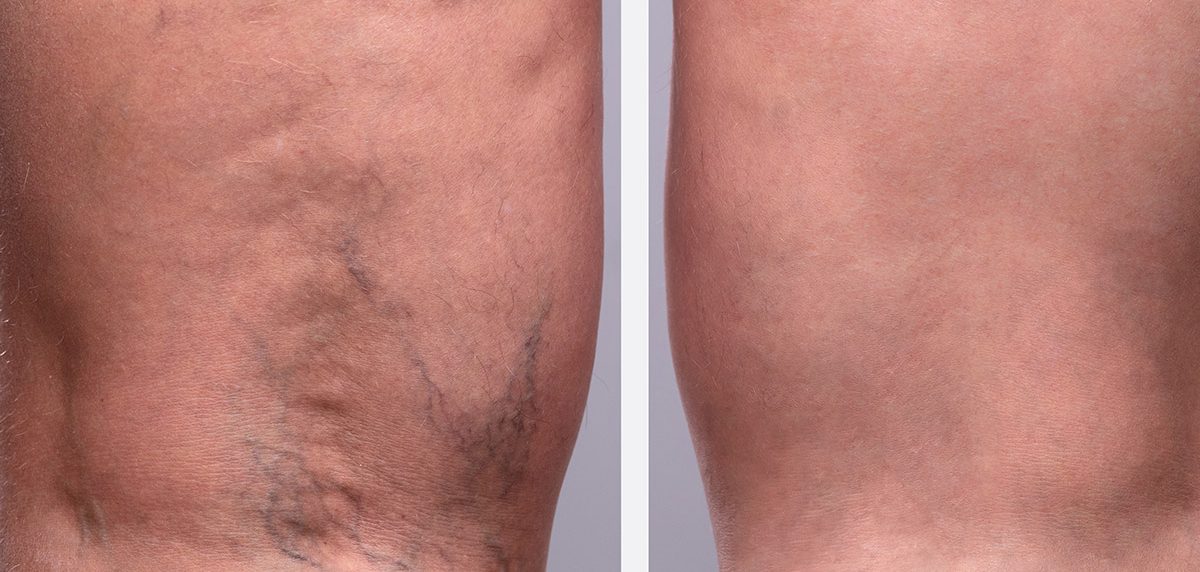
Learn more about how a burning sensation in legs could be a sign of venous disease.
Unless you’ve suffered from it personally, the thought of having varicose veins and spider veins is surely something that would make most people run in the opposite direction. But there are many people who have them without even realizing it, and they need to be treated before they progress any further.
This is because when left untreated, varicose veins can lead to a whole host of other problems. In fact, if you’re reading this article, it’s likely that you have either experienced uncomfortable sensations in your legs or know of someone who has. Perhaps you’ve seen one of our other articles on the topic or are aware of its red flag warning signs: a painful sensation in your legs while standing up, thighs or shins having a burning sensation or increased warmth, and/or itching feeling around your ankles.
Read on to discover everything you need to know about these symptoms, their common causes, as well as how we can treat them at our clinic.
What causes warm sensation in lower leg?
The sensation of warmth or burning in your lower legs can be a sign of many different health conditions. It can also be accompanied by other symptoms or by itself. Here are some of the common causes:
- Blood circulation problems
- Stress and anxiety
- Inflammation of arteries and veins
- Dizziness and fainting spells
- Nerve damage due to diabetes or peripheral arterial disease
- Injuries to the foot or leg
- Prolonged sitting or standing.
What if you have a warm feeling in your lower leg that comes and goes?
If your leg feels hot or you have a warm feeling in your lower leg that comes and goes, you may have blood circulation issues in that area. This can be a sign of deep vein thrombosis (DVT), which is when blood clots form in your leg veins and can travel throughout your body. It is common for the skin to feel warmer in the area where the clot is located and levels of pain vary among those affected. Some patients describe the feeling as a random burning sensation on their skin while others say it feels like fire in their veins. Many patients feel sudden and severe pain in their ankle and/or foot describing that their foot/ankle feels like it’s on fire. Others describe pain in their leg below the knee or a burning sensation in their shins.
If you’re experiencing a burning sensation in your legs while lying down, this can be a sign of DVT as well. A DVT is also known as deep vein thrombosis and can lead to an even more serious condition, pulmonary embolism (PE). A PE is when the blood clot travels to your lungs, which can be life-threatening.
If you’re experiencing any of these symptoms, it’s best to see a doctor as soon as possible so they can examine you and provide treatment.
What is venous disease?
Venous disease is any disease that affects the veins. There are a wide range of diseases that fall under the venous disease umbrella, and each one has its own unique symptoms and treatment needs. A few of the most common venous diseases are varicose veins, spider veins, and DVT/PE.
Varicose veins are swollen, bulging veins that can appear anywhere in the body, but they’re most common in the legs. Spider veins are small, visible veins that tend to appear on the face and chest. Deep vein thrombosis (DVT) and pulmonary embolism (PE) affect the deep veins in your body and can lead to serious health complications if left untreated.
Symptoms of venous disease
Symptoms of venous disease vary depending on the type of vein affected. Some of the more common symptoms include:
- Swelling – Extreme swelling of the legs and feet may be a sign that you have venous disease. This swelling can be both painful and inconvenient, and can make it difficult to fit into shoes or walk.
- Pain – Pain in your leg veins may be one of the first signs of venous disease. Many people with venous disease experience pain in their legs when sitting or standing for long periods of time.
- Cramps – Leg cramps are another common symptom of venous disease. These occur when blood flow through the veins is impaired, causing pain and discomfort in your lower leg and foot.
- Discoloration – In some cases, the skin on your legs may become discolored due to blood stagnation in your veins. This discoloration can range from dark purple to a dark blue-grey and is typically an early warning sign that something may be wrong with your veins.
Risk factors for venous disease
The risk of venous disease increases as the size of the veins diminish, but there is also a connection between vein disease and blood pressure. Blood pressure can have a significant impact on the development of venous disease, and therefore anyone with blood pressure above normal should take special care to protect their veins.
There are many risk factors that contribute to the development of vein disease, including:
Age — As we age, our veins become more fragile and susceptible to damage. Additionally, older body tissue doesn’t heal as quickly and efficiently as younger tissue.
Gender — Women are more likely to develop vein disease than men, due to hormonal differences in the blood. Additionally, women generally have larger veins and therefore more tissue that can be damaged.
Blood Pressure — High blood pressure significantly increases the risk of developing vein disease by damaging blood vessels and altering blood flow patterns. Additionally, diabetics are at a higher risk for developing both chronic leg pain and DVT if their blood pressure is uncontrolled.
Smoking — Smoking accelerates the development of venous disease by damaging blood vessels and reducing blood flow in your legs. It also increases your risk for thrombosis (blood clot) formation in your veins which can lead to DVT.
Obesity — Excess weight in your lower body increases your risk for varicose veins due to increased pressure on your veins from increased body weight. Additionally, individuals who are morbidly obese have an 8x greater risk for DVT than individuals with normal weight and body mass index (BMI).
Treatment for venous disease
There is no a one size fits all treatment for venous disease. The best treatment plan will vary based on the severity of your symptoms, the type of venous disease you have, and your individual overall health.
Although there is no cure for venous disease, there are a number of treatments that can help reduce the discomfort and swelling caused by varicose veins and other venous conditions.
Treatment options may include:
- Lifestyle changes (e.g., exercising regularly, eating healthy foods, and getting enough sleep)
- Compression therapy: These specialized stockings help improve blood circulation in your legs, prevent swelling, and relieve pain. Compression therapy is generally recommended for people with mild to moderate venous disease.
- Surgery: In some cases, surgery may be needed to reduce swelling or track down unusually large veins that are not responding to other treatments.
San Diego Vein Specialists
If you are concerned about your vein health, it’s worth seeing a vein specialist for a consultation.
If you suffer from varicose veins or spider veins, we may recommend considering having a procedure done, such as EVLT, to cure the problem. If you are considering such a procedure, contact Kafri Wellness Clinic to schedule an evaluation and get more information.
At Kafri Wellness Clinic, we have over 25+ years of experience working with patients to address vein issues. We also take into consideration a cardiovascular approach to your treatment to give you as much insight into your health as possible.
If you’d like to schedule a consultation to learn how we can help you, please contact us today!