Deep vein thrombosis (DVT) is a type of blood clot that’s significantly more common in pregnant women and can lead to a more serious condition known as pulmonary embolism (PE). Fortunately, DVT and PE are treatable and even preventable among women who are most at risk. Most mothers with blood clotting conditions have perfectly healthy pregnancies and deliveries.
During pregnancy, up to 90 percent of DVTs occur in the left leg. Early treatment can keep a clot from breaking off and traveling through the circulatory system to the lungs (called a pulmonary embolism, or PE), which can be life-threatening. It can be more likely within six weeks after birth.
What are some significant causes of DVT in postpartum patients?
During childbirth, the body tries to limit bleeding by increasing the level of blood–clotting proteins and decreasing the amount of anti-clotting protein. This can affect all pregnant patients, but particularly occurs with those who have the following:
- An enlarged uterus, which increases pressure on the veins that return the blood to the heart from the lower body.
- Lack of movement due to bed rest.
What signs should postpartum patients look for?
The most common symptoms of deep vein thrombosis during pregnancy and postpartum usually occur in just one leg (most commonly in the left leg) and include:
- A heavy or painful feeling in the leg (a lot of people say that it feels like a really bad pulled muscle that doesn’t go away)
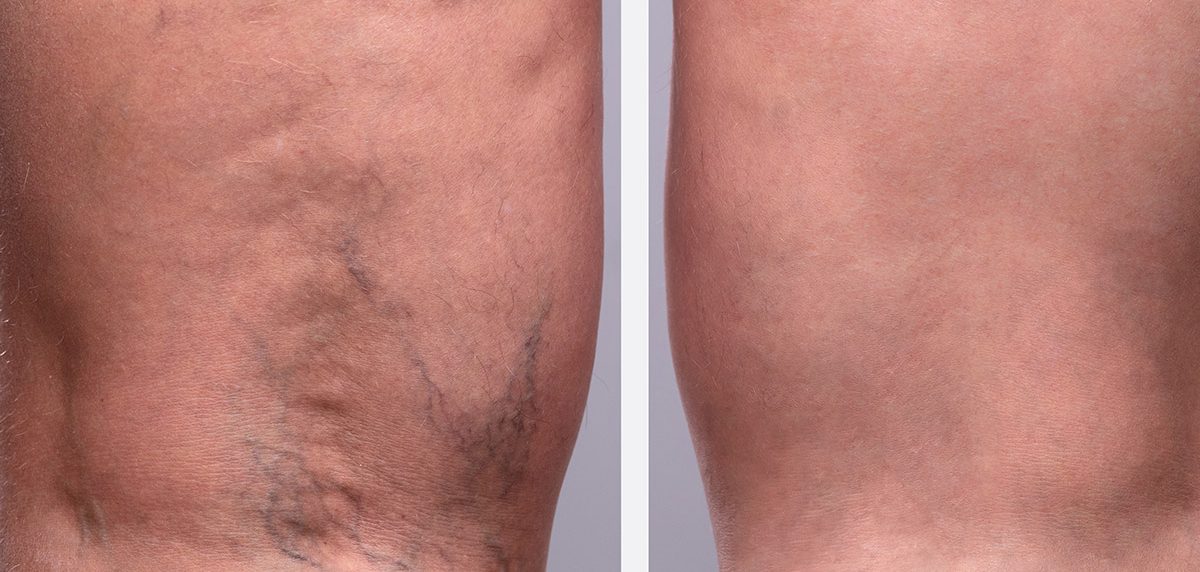
- Tenderness, warmth, and/or redness in the calf or thigh
- Slight to severe swelling
Which postpartum patients are more at risk for DVT?
DVT is more common if you:
- Smoke
- Are on strict bed rest
- Are overweight or obese
- Delivered by cesarean section
- Have a family or personal history of VTE
- Having thrombophilia (an inherited blood clotting disorder)
- Have a postpartum hemorrhage or need a blood transfusion
- Have preeclampsia or certain chronic illnesses including hypertension, diabetes, inflammatory bowel disease, or other vascular diseases
How can you prevent DVT during postpartum?
Be sure to inform your doctor if you have a clotting disorder or if blood clots run in your family. You should also be aware of the signs of a blood clot since early treatment can reduce the risks of complications like PE.
You can help prevent blood clots and DVT by keeping your blood flowing in the following ways:
- Get plenty of pregnancy-safe exercise in, as long as you have the okay from your practitioner.
- Walk and stretch if you’ve been sitting for more than two to three hours. For example, if you’re on a flight or on a long car ride.
- Move your legs while you’re sitting; raise and lower your heels and then your toes.
- Take extra precautions when you travel, including drinking lots of water, getting up frequently to walk or stretching your legs from a seated position.
- If you’re at high risk, your doctor may recommend regularly wearing a support hose. Your practitioner may also prescribe a preventative dose of the blood thinner heparin, or low molecular weight heparin, sometimes during the whole pregnancy or just for several weeks after birth. Both types of medication do not cross the placenta, so they’re safe to take during pregnancy.
Consult with a professional
Some of these symptoms can be severe, but if you receive the help you can avoid complications and severity. If you have a family history of any blood disorders, or experience any alarming symptoms, contact Dr. Kafri’s office immediately. Schedule an appointment by calling or visiting our website for more information.